So, how do you decide which physiotherapist to refer your patients to?
When your patient comes to you and says “yep, I’ve tried physio, it didn’t work” – how do you respond? Do you nod your head knowingly (“yes, physiotherapy can be a bit hit and miss”) or do you look at the letter their physiotherapist has (hopefully!) sent you and understand how they’re hoping you can help, or contact the physiotherapist directly for more information? Do you even know the physiotherapist the patient is talking about? Do you trust that they know what they’re doing? Have they been working with the right physiotherapist for them? And if not, do you know who would be the right physiotherapist for them?
Physiotherapists, like orthopaedic surgeons, SEM doctors, neurosurgeons, rheumatologists, are not all the same (how many times have you come to a different clinical conclusion than a colleague, or revised their work, or been asked for a second opinion!?) Like medicine, physiotherapy is a very broad church. Individual physios have different beliefs, different techniques, different personalities, different skills, different values – and all of those aspects shape how we interact with and treat our patients, and not every physiotherapist will be the right one for the patient sitting in front of you.
Here are some things to consider.
Location
Where does your patient want to be seen – near work, near home, or is location immaterial to them if they find the right physio? My practice is in Liverpool Street, which isn’t going to work for everyone. Most of my patients work in the City but a surprising number are willing to travel – I actually have a few patients who see me fairly regularly, travelling from the south coast, the west country, and Yorkshire, as well as a number from the east coast whose trains come directly into Liverpool Street station.
Price/insurance
Is your patient self-funding, or do they have health insurance? Is the patient very cost-conscious, or are they willing to pay more if they find the right physiotherapist? Do you know a good physio who is able to work with their insurance company? This may be more difficult if the patient is insured with Bupa, Axa, Pru or Aviva, as they tend to be very financially restrictive when it comes to physiotherapy, but other insurers such as Cigna, Allianz and WPA are more focused on quality than price.
Complexity
Is your patient’s condition relatively straightforward (for example, a sprained ankle while playing netball, or low back ache after sitting, with not too many contributing factors) or is it more complicated than that? Do they have a lot going on, lifestyle wise? Do they need a physiotherapist with just the clinical skills to help them recover from their injury, or a physio with life experience who can help them get back on track? Or, if there’s really a lot going on, do they need more of a Sherlock Holmes type approach to work on not just the painful tissue(s) but to see if there’s an underlying cause (posture, sporting technique, previous unresolved issues) – or even a team approach?
Specialism
Some physios specialise in helping patients with specific body parts (eg hand therapist, foot and ankle specialist), specific body systems (eg women’s health), specific stages of life (eg paediatrics), specific jobs (eg musicians or dancers) and others have specific machines (eg ultrasound, shockwave or laser), specific skills (eg joint manipulation, sports rehabilitation, myofascial release, acupuncture) and specific viewpoints (some physios do more hands-on treatment, while others don’t touch their patients and offer exercise-based therapy only). Does your patient need to see a physiotherapist who specialises in one particular area, or do they need to see someone who takes a more holistic, bigger-picture view? Personally – I have taken a lot of courses over the years, and have cherry-picked pieces from many of them, but my overall aim is to use the appropriate skill from the appropriate course with the appropriate patient at the appropriate time, rather than to try to package my patient into any specific protocol.
Experience
Some physios are newly qualified, and others have been qualified for 20 years or more. As is the case in every profession, some of the longer-qualified physios have really reflected on the service they provide and grown over the years, and others have essentially repeated the first year 20 times. Some physios have worked in one clinical area for their whole career, which may make them more expert in that area, but giving them a smaller comfort zone when it comes to patients who don’t quite fit their parameters. Others may have a broader experience, making them potentially less expert in a small area, but giving them a wider understanding of outlying conditions. Having spent my first 10 years as a physiotherapy officer in the Army, with plenty of complex trauma experience, I definitely fall into the latter camp.
Values
For some physios, physiotherapy is a job – they come into work, treat patients and go home – it pays the bills so that they can live the lifestyle they want. For others, like me, it’s a vocation bordering on an obsession. Once a patient comes into our world, we look after them to the best of our ability – we give them the best care we can, researching their issues to find any new evidence, communicating with the other members of their clinical team and introducing new team members where appropriate (different therapists, different experts), making them videos, setting up accountability schedules… whatever is required for the individual to make the best progress. The majority of patients do not need or want this, but for those who do, it’s important that you know that it’s available.
So… location, price, skills, experience and values.
These are all things I try to find out about the consultants I work with (because yes, I fall into that last category, where physiotherapy and patient care are my main focus). So how do I do that? Well, first of all, I look at who’s around, see who looks interesting, or who’s already seeing my patients, and make contact. Lots of the consultants near me run CPD evenings for physios, and I make a point of going to those when I can. From there, I decide whether I want to take the relationship further, and ask to join them in clinic, to watch how they work. I can observe how they interact with the patients, and how they interact with me. If they’re a surgeon, I’ll ask to observe them in theatre. And once I feel confident that I would be happy for this doctor to treat me or my family – then I’ll start referring patients their way.
You cannot know all of these things about all of the physios in all of the areas immediately, or possibly ever – but I believe that if you don’t at least take an interest in who else is treating your patient, then you may not be doing the best possible job for your patients. Not every patient will need it, but for those that do, then knowing and recommending the most suitable physiotherapist is an important part of helping your patients make the best possible recovery.
Why is this so important?
The best patient experiences are built on trust. According to the British Medical Journal, “patients’ trust in their [healthcare professionals] is absolutely fundamental to an effective clinical encounter”.
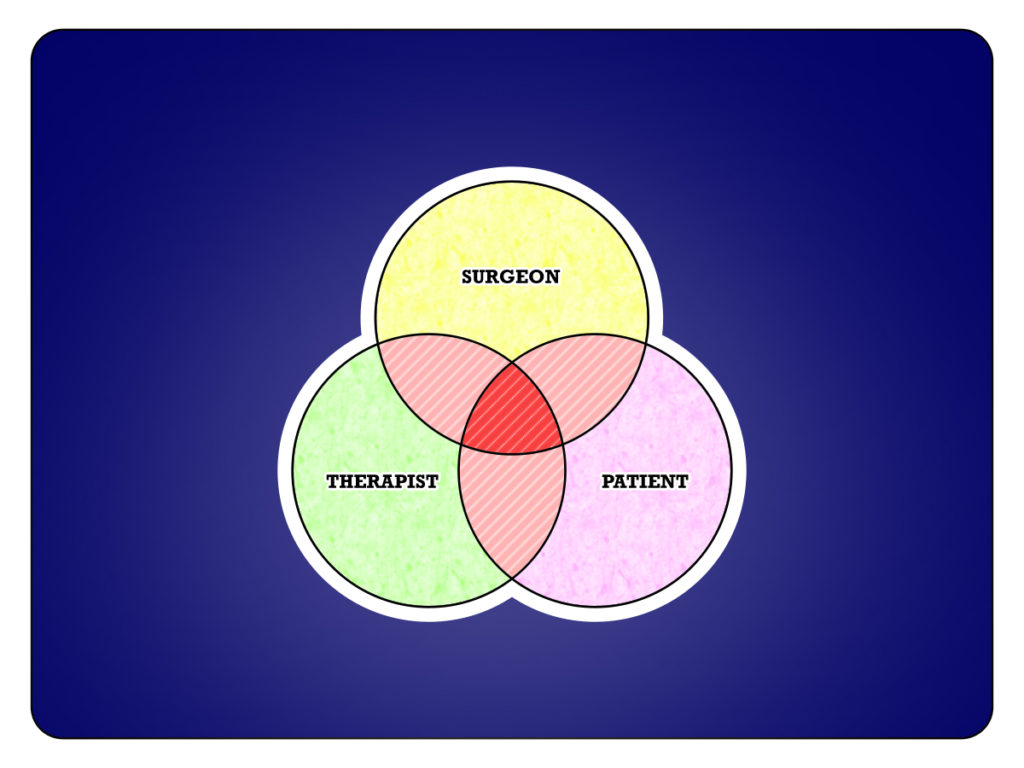
There are three main elements of a great surgical outcome: a great surgeon, a great therapist, and a great patient. And where those three elements overlap, with mutual trust and a shared mission, you find the optimal chance of recovery. Our patients’ belief in us is so important, and the stronger we can build our interdisciplinary clinical relationships, the more we can help each other to ensure the best possible outcome for our patients.
Let’s work together
I would love to help you to get your patients better, so if they have long-term or complex problems, please do send them my way – I have a lot of tools in my “clinical toolbox” and love a challenge.
If you refer a patient to me, my team will be in touch to ask for any information you can give me (such as clinic letters and MRI reports) – or if you prefer to be proactive, please send anything you have to help@nellmead.com where my team will ensure I receive everything in good time to be able to prepare.
If you are happy to discuss the case in person or over the phone, please just let my team know and we will make this happen.
I also love to get to know the other members of my patients’ teams, so if we do not already know each other when you refer a patient to me, I will probably ask to get in touch and ideally visit you in clinic or in theatre, and/or meet up for a coffee. Alternatively, you are very welcome to visit me, with or without our mutual patient! I believe that the better we know and trust each other, the more effectively we can help our patients.
Get in touch to tell me about your patient, and let’s get started.
