One of the things I really love about Diane and LJ is how they adapt to change…
Over the past few weeks, I’ve been writing about Diane Lee’s Integrated Systems Model (ISM), which is a big part of how I work. I’ve explained how I found Diane, how the ISM works with the published evidence, and the theory of regional interdependence from which the ISM derived. As everyone’s body and movement patterns are (and should be) different, I then wrote about the meaning of optimal movement as opposed to suboptimal movement with areas of failed load transfer (FLT). We went through how we assess for FLTs during screening tasks, corrected his impairments to find our driver, and then found the vectors. Finally, we identified the underlying system impairment and created a treatment plan for our fictional patient, David.
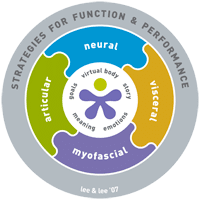
One of the things I haven’t mentioned is the Clinical Puzzle. It’s a tool that Diane and LJ built to help therapists work out why our patients are struggling, and it’s a graphical representation of the various elements of the ISM:
• Meaningful complaint – what is the patient’s symptom?
• Meaningful task – what are they doing when they experience the symptom?
• Screening tasks – what are the building blocks of the meaningful task, that we will use to test the patient to find their driver?
• Where are their areas of failed load transfer (FLT) in each screening task?
• Which are the underlying system impairments, as found on vector analysis?
• Are there any cognitive or emotional barriers to treatment?
When I first did the Series in 2013 (the six-month intensive mentorship for physios who want to really understand the ISM and incorporate it into their daily practice), both Diane and LJ were using the Clinical Puzzle heavily. It wasn’t where they would write all their session notes (there isn’t room on the puzzle for everything I learn in a 90-minute assessment session!) but it acted as their aide-memoire to clinical reasoning.
Confession: much as I love the phrase “clinical puzzle,” as that represents every patient I’ve ever met, I’ve never liked the graphic. My brain works in a much more linear way, and while we had to use the puzzle to write the essays and case studies that were a part of the course, I certainly wasn’t using it in everyday practice – it just felt like an extra faff – and I still don’t.
So I was very relieved when I went to do LJ’s Part 4 course in 2017, and Diane’s update course in 2018 (their business partnership ended in 2013 as they both wanted different things from life), to find that neither of them is really using the puzzle any more! I guess it was one of those things that makes sense to start with, or at least makes more sense than anything else you can come up with, but that doesn’t stand the test of time. And one thing I really appreciate about both LJ and Diane is that if a thing doesn’t work, they don’t stick with it blindly, they go ahead and change it for something better.
Instead, LJ now uses a series of tables to note all the FLTs and what happens to them; and Diane has created a flow chart that she feels simplifies the reasoning process. It will be interesting to see how these develop over time, and what any future iterations will bring!

